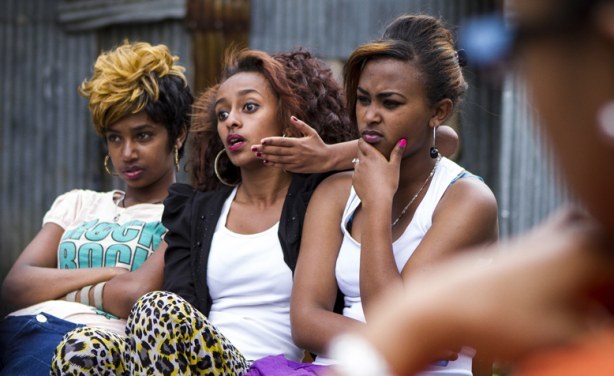
Photo: Sheikh Rajibul Islam/duckrabbit
Teenagers discussing sex at a youth group during the International Family Planning Conference in Addis Ababa, Ethiopia.
Johannesburg — The life of a teenager is difficult enough without the added burden of living with HIV, keeping it hidden from friends and sticking to antiretroviral treatment.
But new data has revealed that while AIDS-related deaths globally have fallen in the general population over the last seven years, deaths among adolescents rose by 50 percent in the same period and UN agencies are raising the alarm.
The World Health Organization (WHO) blames the high number of deaths on the “poor prioritization” of teenagers in national HIV plans; inadequate HIV services, and lack of support for adolescents to remain in care and stick to antiretroviral therapy (ART).
With a generation of children who were born HIV-positive now reachingyoung adulthood, countries in sub-Saharan Africa can no longer slot young people into paediatric programmes or even adult health facilities.
WHO has released new guidelines that, for the first time, address the specific needs of adolescents living with HIV as well as those at risk of infection. More than 2 million adolescents between the ages of 10 and 19 years are living with HIV.
“Adolescents face difficult and often confusing emotional and social pressures as they grow from children into adults. Adolescents need health services and support tailored to their needs. They are less likely than adults to be tested for HIV, and often need more support than adults to help them maintain care and to stick to treatment,” said Dr Gottfried Hirnschall, Director of the WHO HIV/AIDS Department.
According to WHO, only 10 percent of young men and 15 percent of young women between 15 and 24 years in sub-Saharan Africa know their HIV status, while access to HIV testing and counselling in other regions is consistently reported as being very low.
In addition, adolescents born with HIV are often being diagnosed late, and start treatment only when they are already very ill.
A major barrier is that in some countries adolescents need their parents’ consent to get tested and WHO recommends that governments review their laws to make it easier for adolescents to obtain HIV testing without parental consent.
In South Africa, for example, different threshold ages of consent apply to HIV-related services such as treatment, voluntary medical male circumcision, contraception, and HIV testing. Consent for an HIV test may be given by a child who is 12 years or older, and also by a child under the age of 12 if they are “of sufficient maturity to understand the benefits, risks and social implications of such a test”.
Nicola Willis, director of Zvandiri, an organization providing community-based treatment, care and support for adolescents living with HIV, suggests that more needs to be done at community level to engage families and make them realise the importance of getting young people tested.
“We’ve seen 14 year olds waiting till they are very sick to get tested, and it can often be too late,” she noted.
Botswana was among the first countries in southern Africa to provide free antiretroviral drugs, and the experience of the Botswana-Baylor Children’s Clinical Center of Excellence in treating and supporting HIV-positive adolescents helped to inform the WHO guidelines.
Dr Gabriel Anabwani, director of the Baylor clinic in Botswana, relates how when the centre began treating HIV-positive children in 2001, they found that the kids were not adhering to their ARV treatment because they had not been told what their HIV status was.
“Some children were just told that the pills were for a cough, so when the cough stopped, they would stop taking the medicines… others were told that the pills are for children that have lost their parents … [the] children didn’t understand why they have to take this medication, and when will it ever stop,” he told IRIN.
The situation improved when the clinic decided to involve both parents in disclosing the child’s status and in adherence to medication. But when the children become adolescents, the parents assume they are old enough to take their medication on their own, and adherence rates plummet.
A typical teenager – HIV-positive or not – generally won’t like being told they have to take medicine for the rest of their life; they are likely to be sexually active, and if they are positive, may not have disclosed their status to their partner. They are usually away from home more, and sometimes depressed because of their HIV status. “With all this going on, many begin to die from AIDS-related complications, such as TB,” Anabwani said.
The mental health needs of young people living with the virus are still overlooked, Willis noted.
In the guidelines, WHO notes that health worker training on HIV-related services for adolescents “needs urgent attention” and should focus particularly on mental health, disclosure and treatment.
Peer support is an effective coping strategy. In Zimbabwe, Zvandiri has trained and mentored HIV-positive teens to work in communities and clinics, providing adherence support to children on treatment.
Botswana’s Baylor clinic has created support groups or “teen clubs” for adolescents on treatment, a best practice model that has been replicated in other countries in the region.
“You could be the best counsellor in the world, but you will never be as effective as a peer in encouraging and motivating youth to adhere,” Willis told IRIN.
[This report does not necessarily reflect the views of the United Nations.]